Quantitative lung ultrasound spectroscopy: First comparison with gold standard computed tomography scan and standard lung ultrasound for diagnosis of pneumonia versus cardiogenic pulmonary edema
Keywords:
Cardiogenic pulmonary edema, computed tomography, lung ultraound, pneumonia, quantitative lung ultrasoundAbstract
Background: Pneumonia (PNE) and cardiogenic pulmonary edema (CPE) are characterized by reduced air-spaces dimension and edema. Their distinction through gold standard computed tomography (CT) is challenging due to their pattern similarity. Lung Ultrasound (LUS) is a tool for monitoring the progression of lung pathologies. LUS is portable, real-time, and non-ionized; however, standard LUS (S-LUS) relies on the subjective visualization of imaging patterns, leading to poor reproducibility and lack of diagnostic specificity. To enhance LUS diagnostic utility, quantitative LUS (Q-LUS) was developed. Q-LUS quantifies imaging patterns and explores their correlation to different pathophysiological conditions. In literature, vertical artifacts (VA) quantification proved capable of differentiating PNE and CPE, however, this approach was never compared with gold standard.
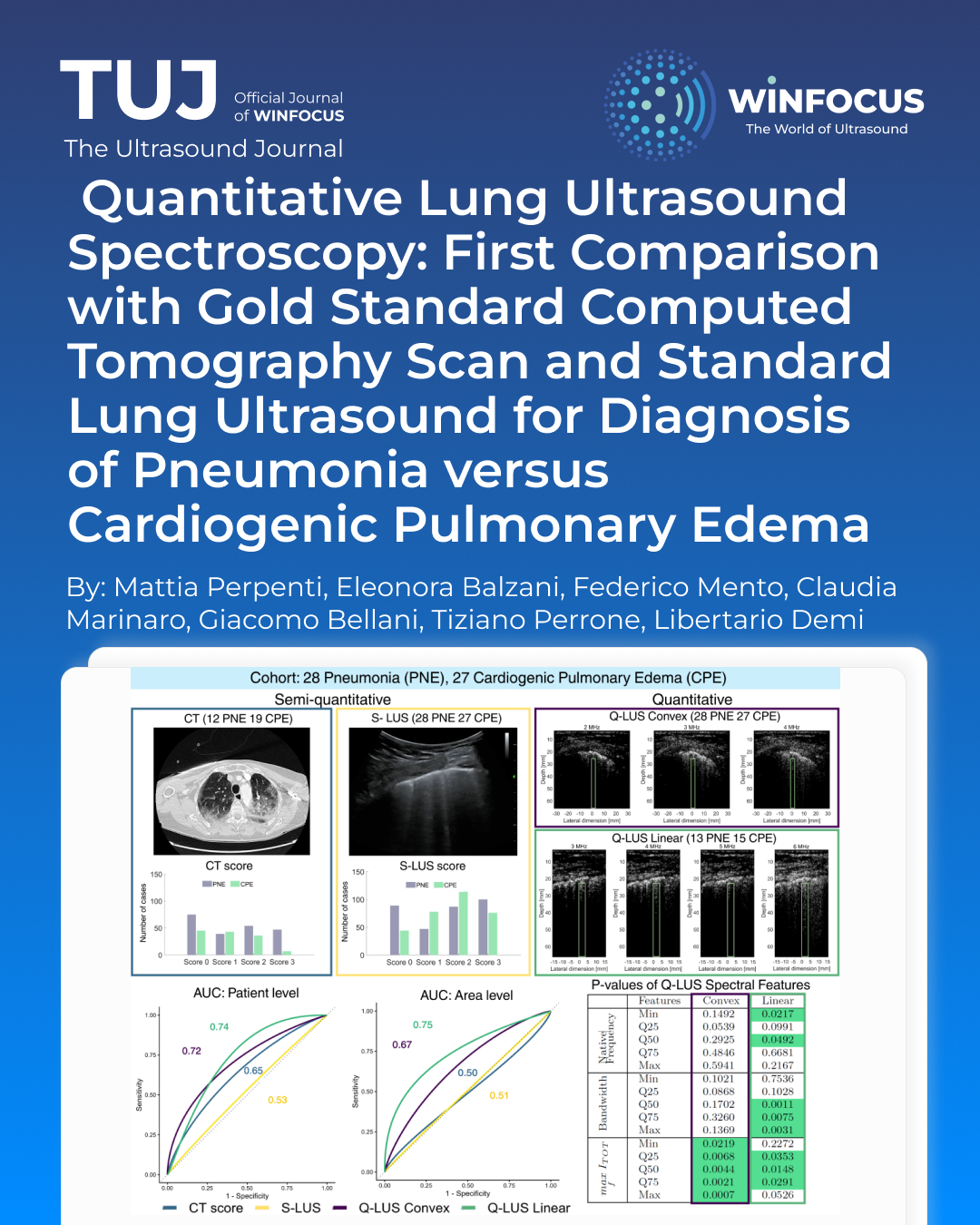
Methods: We statistically investigate and compare the clinical significance of CT, S-LUS, and Q-LUS, in differentiating PNE and CPE. From a cohort of 55 patients, CT, S-LUS, and Q-LUS data are acquired. CT and S-LUS data of each patient are evaluated to assign a semi-quantitative CT-score and S-LUS-score. Q-LUS radiofrequency data are acquired in multifrequency with convex (2, 3, and 4 MHz) and linear (3, 4, 5, and 6 MHz) probes. VA are manually segmented, quantified into three spectral quantities, and statistically analyzed to extract 15 features for each patient. The diagnostic significance of the scores is tested through Generalized Estimating Equation models.
Results & Conclusions: Results show areas under the curve of 74%, 72%, 65%, and 53% for Q-LUS linear, Q-LUS convex, CT-score, and S-LUS-score, respectively, highlighting Q-LUS as the most significant tool.
References
1. Matthay MA, Zemans RL, Zimmerman GA, Arabi YM, Beitler JR, Mercat A, et al. Acute respiratory distress syndrome. Nat Rev Dis Primers 2019;5:18 doi:10.1038/s41572-019-0069-0
2. Mazzon E, Cuzzocrea S. Role of TNF-alpha in lung tight junction alteration in mouse model of acute lung inflammation. Respir Res 2007;8:75 doi:10.1186/1465-9921-8-75
3. Brito R, Lucena-Silva N, Torres L, Luna C, Correia J, da Silva G. The balance between the serum levels of IL-6 and IL-10 cytokines discriminates mild and severe acute pneumonia. BMC Pulm Med 2016;16:170 doi:10.1186/s12890-016-0324-z
4. Ware LB, Fremont RD, Bastarache JA, Calfee CS, Matthay MA. Determining the etiology of pulmonary edema by the edema fluid-to-plasma protein ratio. Eur Respir J 2009;35:331-7 doi:10.1183/09031936.00098709
5. Suciadi L, Pranata R, Huang I, Lim MA, Yonas E, Henrina J, et al. Comparing lung CT in COVID-19 pneumonia and acute heart failure: an imaging conundrum. Cureus 2021;13:e15120 doi:10.7759/cureus.15120
6. Mento F, Demi L. Dependence of lung ultrasound vertical artifacts on frequency, bandwidth, focus and angle of incidence: an in vitro study. J Acoust Soc Am 2021;150:4075-82 doi:10.1121/10.0007482
7. Al Deeb M, Barbic S, Featherstone R, Dankoff J, Barbic D. Point-of-care ultrasonography for the diagnosis of acute cardiogenic pulmonary edema in patients presenting with acute dyspnea: a systematic review and meta-analysis. Acad Emerg Med 2014;21:843-52 doi:10.1111/acem.12435
8. Demi L, Wolfram F, Klersy C, De Silvestri A, Ferretti VV, Muller M, et al. New international guidelines and consensus on the use of lung ultrasound. J Ultrasound Med 2022;42 doi:10.1002/jum.16088
9. Mento F, Khan U, Faita F, Smargiassi A, Inchingolo R, Perrone T et al. State of the art in lung ultrasound, shifting from qualitative to quantitative analyses. Ultrasound Med Biol 2022;48:2398-416 doi:10.1016/j.ultrasmedbio.2022.07.007
10. Mento F, Perini M, Malacarne C, Demi L. Ultrasound multifrequency strategy to estimate the lung surface roughness, in silico and in vitro results. Ultrasonics 2023;135:107143 doi:10.1016/j.ultras.2023.107143
11. Perpenti M, Mento F, Pierro G, Perrotta A, Perrone T, Smargiassi A, et al. Fully automated quantitative lung ultrasound spectroscopy for the differential diagnosis of lung diseases: the first multicenter in-vivo clinical study. Comput Biol Med 2026;200:111365 doi:10.1016/j.compbiomed.2025.111365
12. Mento F, Perpenti M, Barcellona G, Perrone T, Demi L. Lung ultrasound spectroscopy applied to the differential diagnosis of pulmonary diseases: an in vivo multicenter clinical study IEEE Trans Ultrason Ferroelectr Freq Control 2024;71:1217-32 doi:10.1109/TUFFC.2024.3454956
13. Mento F, Perpenti M, Barcellona G, Perrone T, Demi L. Quantitative lung ultrasound spectroscopy classification performance in differentiating CPE, pneumonia, and PF: a comparative classifiers’ analysis. IEEE Trans Ultrason Ferroelectr Freq Control 2024:1-4 doi:10.1109/UFFC-JS60046.2024.10793564
14. Smargiassi A, Soldati G, Torri E, Mento F, Milardi D, Del Giacomo P et al. Lung ultrasound for COVID-19 patchy pneumonia. J Ultrasound Med 2021;40:521-8 doi:10.1002/jum.15428
15. Mento F, Perrone T, Macioce VN, Tursi F, Buonsenso D, Torri E. On the impact of different lung ultrasound imaging protocols in the evaluation of patients affected by coronavirus disease 2019: how many acquisition do we need? J Ultrasound Med 2021;40:2235-8 doi:10.1002/jum.15580
16. Soldati G, Smargiassi A, Inchingolo R, Buonsenso D, Perrone T, Briganti DF, et al. Proposal for international standardization of the use of lung ultrasound for COVID-19 patients: a simple, quantitative, reproducible method J Ultrasound Med 2020;39 doi:10.1002/jum.15285
17. Mento F, Perrone T, Fiengo A, Tursi F, Macioce V. N., Smargiassi A, et al. Limiting the areas inspected by lung ultrasound leads to an underestimation of COVID-19 patients’ condition. Intensive Care Med 2021;47 doi:10.1007/s00134-021-06407-0
18. Mento F, Perrone T, Fiengo A, Smargiassi A, Inchingolo R, Soldati G, et al. Deep learning applied to lung ultrasound videos for scoring COVID-19 patients: a multicenter study. J Acoust Soc Am 2021;149:3626-34 doi:10.1121/10.0004855
19. Demi L, Mento F, Di Sabatino A, Fiengo A, Sabatini U, Macioce VN, et al. Lung ultrasound in COVID-19 and post-COVID-19 patients, an evidence-based approach. J Ultrasound Med 2022;41:2203-15 doi:10.1002/jum.15902
20. Tortoli P, Bassi L, Boni E, Dallai A, Guidi F, Ricci S. ULA-OP: an advanced open platform for ultrasound research. IEEE Trans Ultrason Ferroelectr Freq Control 2009 doi:10.1109/TUFFC.2009.1303
21. Jalilian H, Afrakhteh S, Mento F, Zannin E, Rigotti C, Cattaneo F, et al. Lung ultrasound video scoring using a novel motion-aware segmentation technique: toward automated neonatal LUS scoring. Comput Biol Med 2025;198:111244 doi:10.1016/j.compbiomed.2025.111244
22. Soldati G, Demi M, Smargiassi A, Inchingolo R, Demi L. The role of ultrasound lung artifacts in the diagnosis of respiratory diseases. Expert Rev Respir Med 2019;13:163-72 doi:10.1080/17476348.2019.1565997
23. Mento F, Soldati G, Prediletto R, Demi M, Demi L. Quantitative lung ultrasound spectroscopy applied to the diagnosis of pulmonary fibrosis: first clinical study. IEEE Trans Ultrason Ferroelectr Freq Control 2020:1-1 doi:10.1109/TUFFC.2020.3012289
24. Perpenti M, Mento F, Afrakhteh S, Barcellona G, Perrone T, Demi L. A novel empirical wavelet transform approach for classification of radiofrequency lung ultrasound signals applied to diagnosis of lung diseases. IEEE Trans Ultrason Ferroelectr Freq Control 2024:1-4 doi:10.1109/UFFC-JS60046.2024.10793884
25. Demi L, van Hoeve W, van Sloun R. J. G., Soldati G, Demi M. Determination of a potential quantitative measure of the state of the lung using lung ultrasound spectroscopy. Sci Rep 2017;7:12746 doi:10.1038/s41598-017-13078-9
26. Perpenti M, Mento F, Pierro G, Perrotta A, Smargiassi A, Inchingolo R, et al. Novel quantitative lung ultrasound spectroscopy approach for diseases classification. IEEE Trans Ultrason Ferroelectr Freq Control 2024:1-4 doi:10.1109/UFFC-JS60046.2024.10793543
27. Hopewell S, Chan A-W, Collins GS, Hróbjartsson A, Moher D, Schulz KF, et al. CONSORT 2025 explanation and elaboration: updated guideline for reporting randomised trials. BMJ 2025;389 doi:10.1136/bmj-2024-081124
28. Padrao E M H, Caldeira A B, Gardner T A, Miyawaki I A, Gomes C, Riceto L J, et al. Lung ultrasound findings and algorithms to detect pneumonia: a systematic review and diagnostic testing meta-analysis. Crit Care Med 2025;53 doi:10.1097/CCM.0000000000006818
29. Staub L J, Biscaro R R M, Kaszubowski E, Maurici R. Lung ultrasound for the emergency diagnosis of pneumonia, acute heart failure, and exacerbations of COPD/asthma in adults: a systematic review and meta-analysis. J Emerg Med 2018;56 doi:10.1016/j.jemermed.2018.09.009
30. Chiumello D, Mongodi S, Algieri I, Vergani G L, Orlando A, Via G, et al. Assessment of lung aeration and recruitment by CT scan and ultrasound in acute respiratory distress syndrome patients. Crit Care Med 2018;46:1 doi:10.1097/CCM.0000000000003340
31. Akor E A, Gao J, Guo J, Han B, Cruz A F, Herrmann J, et al. Structural and functional characteristics of healthy and injured porcine lungs during deflation: a quantitative CT imaging analysis. J Appl Physiol (1985) 2025;138:1615-27 doi:10.1152/japplphysiol.00443.2024
Downloads
Section
License
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by-nc/4.0) which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Authors retain the copyright for their published work. No formal permission will be required to reproduce parts (tables or illustrations) of published papers, provided the source is quoted appropriately and reproduction has no commercial intent.











